What Is Deep Vein Thrombosis?
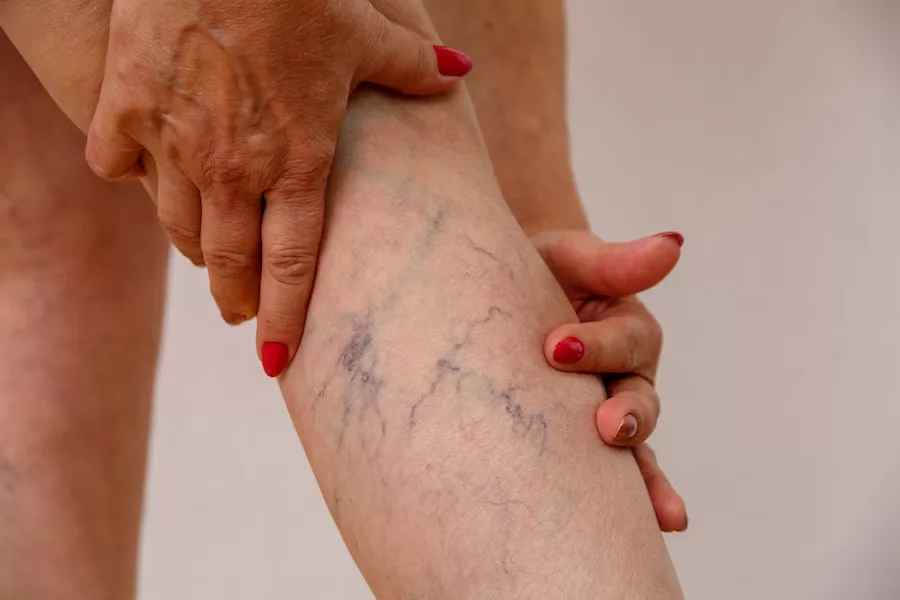
The circulatory system of the leg comprises arteries and veins, where arteries transport blood from the heart to the limbs, and veins carry it back to the heart. In the leg, there are both superficial veins, located near the surface, and deep veins, situated deeper within the limb. Deep vein thrombosis (DVT) is a condition characterized by the formation of a blood clot, also known as a thrombus, within a deep vein. While DVTs are most commonly found in the veins of the leg, specifically the calf or thigh, they can also develop in other areas of the body.
DVT is a potentially life-threatening medical emergency. If a clot dislodges and travels through the bloodstream, it can become lodged in the lung, leading to a condition known as a pulmonary embolism. This blockage in the lung can severely impair breathing and, in some cases, prove fatal. Clots in the thigh are more likely to result in a pulmonary embolism than those in the calf.
Causes of DVT
Numerous factors contribute to the formation of DVT, and the presence of multiple risk factors increases the likelihood of experiencing a DVT. Nevertheless, even individuals without these risk factors can develop DVT.
Risk Factors for DVT:
Blood or vein-related conditions:
- Previous DVT
- Varicose veins
- Blood clotting disorders
- Family history of DVT or blood clotting disorders
Other medical conditions:
- Heart disease
- Chronic swelling of the legs
- Obesity
- Inflammatory bowel disease
- Cancer
- Dehydration
- Sepsis
Women’s health factors:
- Hormone replacement therapy
- Birth control pills containing estrogen
- Pregnancy or recent childbirth
Other factors:
- Age over 40 years old
- Immobility (due to inactivity or cast-wearing)
- Recent surgery
- Trauma (injury)
- Smoking
Signs and Symptoms of DVT in the Leg
Some individuals with DVT in the leg may exhibit either no warning signs or very vague symptoms. It is essential to consult a doctor for evaluation if any of the following warning signs or symptoms are present:
- Swelling in the leg
- Pain in the calf or thigh
- Warmth and redness of the leg
Diagnosis
Diagnosing DVT can be challenging, especially when the patient is asymptomatic. Furthermore, the similarity between DVT symptoms and those of other conditions, such as muscle strains, infections, superficial vein clots (thrombophlebitis), fractures, or arthritis, can complicate the diagnosis. If DVT is suspected, the doctor will promptly refer the patient to a vascular laboratory or a hospital for testing, which may involve blood tests, Doppler ultrasound, venography, MRI, or angiography.
Treatment of DVT
Upon confirmation of a clot’s presence, the doctor will recommend an appropriate treatment plan. Hospitalization may be necessary depending on the clot’s location. A multidisciplinary team of physicians, which may include a primary care physician, internist, vascular surgeon, or hematologist, will manage medical or surgical care.
Treatment options may encompass:
- Medication: Typically, blood-thinning medications are prescribed to prevent the formation of additional clots.
- Compression stockings: Wearing fitted hosiery helps reduce pain and swelling.
- Surgery: A vascular specialist may perform a surgical procedure if required.
Complications of DVT
An early and exceptionally serious complication of DVT is the development of a pulmonary embolism. This occurs when the clot dislodges and migrates to the lung. Symptoms of a pulmonary embolism include:
- Shortness of breath
- Chest pain
- Coughing up blood
- A sense of impending doom
Long-term consequences of DVT include damage to the affected vein, leading to persistent swelling, pain, and discoloration of the leg.
Preventive Measures
For individuals with risk factors for DVT, these strategies may help reduce the likelihood of developing a blood clot:
- Adhere to prescribed blood-thinning medications.
- Mitigate modifiable risk factors, such as quitting smoking and maintaining a healthy weight.
- During prolonged periods of immobility, such as on long journeys:
- Exercise the legs every two to three hours to facilitate blood circulation back to the heart.
- Engage in activities like walking up and down the aisle on a plane or train, rotating ankles while seated, and taking regular breaks during road trips.
- Stay well-hydrated by drinking ample fluids while avoiding alcohol and caffeine.
- Consider using compression stockings.